PRP for Chronic Joint Pain: What the Evidence Shows
Short Answer
- PRP (platelet-rich plasma) injections can help chronic joint pain
- PRP uses concentrated growth factors from your own blood to support tissue repair in damaged joints
- Published research and our patient outcome registry show most patients experience meaningful improvement in pain and function within 4 to 12 weeks, with benefits lasting 12 months or longer
If you have been told "there is nothing else we can do," or your cortisone injections have stopped working, or you are trying to avoid surgery for a joint that keeps getting worse, you are not alone. That is exactly the situation most of our patients were in before they found us. The common thread is that no one identified the specific tissue generating the pain, and that missing step is the most common reason previous treatments have not produced lasting relief.
Platelet-rich plasma (PRP) is a treatment that uses a concentrated preparation of platelets from your own blood, containing growth factors that support tissue repair, injected directly into damaged joints under image guidance. If you have been dealing with ongoing joint pain that has not responded to physical therapy, medications, or steroid injections, PRP may offer a different path forward.
At Regenerative Performance in Gilbert, Arizona, PRP injections are performed by Dr. Drew Timmermans, a naturopathic physician and Registered Musculoskeletal Sonographer (RMSK), for patients with chronic joint conditions due to knee osteoarthritis, rotator cuff injuries, hip labral tears, and tendon or ligament damage. Every injection is ultrasound-guided or fluoroscopy-guided because the proper diagnosis determines the outcome, and accuracy directly impacts results.
This page covers why chronic joint pain persists, what PRP is, how it works at the tissue level, what current research shows, and what to expect if you are considering treatment at our clinic.
If you have chronic joint pain that hasn't improved with PT, chiropractic, or cortisone, the next step is a detailed, in-person assessment to identify the exact tissues causing your pain and review non-surgical orthobiologic options like PRP and Stem Cell Therapy.
Schedule a comprehensive 2-hour evaluation for your chronic joint pain at our Gilbert, AZ clinic (also serving Chandler, Mesa, Queen Creek, and the greater Phoenix area).
Key Facts About PRP Therapy
- What PRP is: A concentrated preparation of your own platelets, containing growth factors that support tissue repair
- How it works: PRP delivers growth factors directly to damaged tissue, modulating inflammation and stimulating the body's repair processes
- Clinical outcomes: Across 376 tracked cases over five years at Regenerative Performance, 76.9% of patients achieve clinically meaningful pain relief and 76.8% achieve meaningful improvement in daily function
- Safety profile: Because PRP uses your own blood, the risk of adverse reaction is very low
- Treatment timeline: Most patients notice gradual improvement over 4 to 12 weeks as tissue repair progresses
- Cost transparency: PRP is not covered by insurance. We provide detailed pricing during your evaluation so there are no surprises
- Next step: Call 480-508-4226 to schedule a 2-hour evaluation for chronic joint pain in Gilbert, AZ
Why Does Chronic Joint Pain Get Worse Over Time?
Chronic joint pain develops when tissue breakdown triggers a self-perpetuating cycle of inflammation and further damage that traditional treatments only interrupt temporarily. Understanding this cycle helps explain why your previous treatments may not have produced lasting relief, and why a different approach may be needed.
The Cartilage Story
One common pathway starts with cartilage, the smooth tissue covering joint surfaces. Cartilage begins to break down from injury, repetitive stress, or age-related changes. As it thins, the underlying bone loses its protective cushion. This triggers an inflammatory cascade: the joint lining (synovium) becomes inflamed, producing excess fluid and inflammatory mediators that further accelerate cartilage breakdown while sensitizing pain receptors.
Over time, this cycle becomes self-perpetuating: inflammation drives tissue breakdown, which drives more inflammation. As cartilage loss progresses, increased mechanical loading on the subchondral bone can cause bone marrow edema, another significant source of pain that often goes undiagnosed.
Beyond Cartilage: The Whole Joint
But cartilage is not the only pain driver. Many patients have chronic joint pain with perfectly intact cartilage. Tendons and ligaments around the joint can become damaged from overuse, injury, or chronic inflammation. Joint misalignment can overstretch ligaments and create ongoing mechanical stress. Peripheral nerves running near the joint can become irritated or entrapped, contributing their own pain signals.
This is an important distinction because most clinics focus exclusively on what is happening inside the joint. At our practice, we evaluate and treat the entire joint complex: cartilage, tendons, ligaments, nerves, and subchondral bone. Treating only one structure while ignoring the others often explains why previous treatments have failed.
Traditional treatments like anti-inflammatory medications and steroid injections can interrupt the inflammatory cycle temporarily but do not address the underlying tissue damage in any of these structures.
There is growing evidence that repeated steroid injections may actually accelerate cartilage loss. A landmark 2017 randomized trial published in JAMA found that patients receiving corticosteroid injections every three months for two years lost significantly more cartilage than patients receiving saline, with no superior pain relief (McAlindon et al., JAMA, 2017). If your current treatment path involves repeated cortisone injections, the research suggests it may be making the underlying problem worse.
This is where regenerative approaches like PRP differ. Rather than simply blocking inflammation or masking pain signals, PRP delivers biological signals that support actual tissue repair across all of these tissue types.
What Is PRP Treatment?
PRP is a concentrated preparation of platelets from your own blood that delivers growth factors directly to damaged tissue to support repair. It is not a drug or a synthetic product. It is your own biology, concentrated and redirected to where it is needed most.

Platelet-rich plasma is exactly what the name describes: a concentration of platelets derived from your own blood that contains a higher-than-normal level of growth factors and signaling proteins.
During preparation, a blood sample is drawn and processed in a centrifuge to separate the platelet-rich layer from other blood components. The resulting PRP preparation typically contains 3 to 10 times the normal concentration of platelets found in whole blood, and sometimes higher depending on the clinical application.
These platelets contain granules packed with growth factors including platelet-derived growth factor (PDGF), vascular endothelial growth factor (VEGF), transforming growth factor beta (TGF-B), and insulin-like growth factor (IGF-1). When injected into damaged tissue, these growth factors initiate and support the biological repair process.
How Do PRP Injections Work?
PRP works on multiple fronts: delivering growth factors, calming inflammation, improving joint lubrication, and dialing down pain signals. It works through several complementary mechanisms that address different aspects of joint damage and pain.
Growth Factor Delivery
The primary mechanism of PRP is direct delivery of concentrated growth factors to damaged tissue. PDGF stimulates cell proliferation and new blood vessel formation. VEGF supports the development of new blood supply to injured areas. TGF-B promotes tissue remodeling and collagen production. IGF-1 stimulates cell growth and differentiation.
Together, these growth factors create a biological environment that supports tissue repair rather than just managing symptoms.
Inflammation Modulation
Unlike steroid injections that suppress all inflammation (including the beneficial inflammatory processes needed for healing), PRP modulates the inflammatory response. It shifts the joint environment from chronic, destructive inflammation toward the controlled inflammatory response that characterizes normal tissue repair.
This distinction matters because some inflammation is necessary for healing. Steroids eliminate inflammation entirely, which provides short-term relief but may impair the joint's ability to heal itself.
Joint Lubrication and Synovial Health
PRP appears to improve the quality of synovial fluid, the natural lubricant in your joints. Healthier synovial fluid reduces friction between joint surfaces and provides better nutrient delivery to cartilage.
For patients with osteoarthritis, where synovial fluid quality degrades significantly, this effect can contribute to improved joint function and reduced pain during movement.
Treating the Structures Around the Joint
As discussed above, joint pain often originates from multiple structures, not just cartilage. PRP can be delivered precisely to damaged tendons, partially torn ligaments, irritated peripheral nerves, and areas of subchondral bone edema. This comprehensive approach is why image-guided injection matters: we need to place PRP exactly where the damage is, and that often means treating three or four structures in a single session.
Pain Signal Reduction
Beyond tissue repair, PRP appears to directly influence pain signaling in the joint. Research suggests PRP can reduce the concentration of pain-mediating chemicals in the joint environment and may modulate how pain signals are transmitted from the joint to the nervous system.
This helps explain why some patients report pain improvement before structural changes would be expected to occur.
Schedule a comprehensive 2-hour evaluation for your chronic joint pain at our Gilbert, AZ clinic.
What Does the Research Say About PRP for Joint Pain?
A 2024 meta-analysis found PRP produced statistically significant superiority over hyaluronic acid, corticosteroids, and saline for knee osteoarthritis, with published evidence of benefits sustained at 18 months and even 5 years. The evidence base for PRP has grown substantially over the past decade. A 2024 meta-analysis published in the American Journal of Sports Medicine analyzed randomized controlled trials and found that PRP demonstrated statistically significant superiority over hyaluronic acid, corticosteroids, and saline for knee osteoarthritis pain and function outcomes (Oeding et al., Am J Sports Med, 2024). Earlier meta-analyses have shown benefits lasting 12 months or longer.
Research also supports PRP effectiveness across multiple musculoskeletal conditions. Randomized controlled trials have demonstrated positive outcomes for partial-thickness rotator cuff tears (Tanpowpong et al., Sports Med Open, 2023), plantar fasciitis (Kumar et al., Cureus, 2024), hip osteoarthritis (Nouri et al., BMC Musculoskelet Disord, 2022), and even carpal tunnel syndrome (Malahias et al., J Tissue Eng Regen Med, 2018). A 2024 dose-response meta-analysis confirmed that higher platelet concentrations correlate with better outcomes across musculoskeletal conditions (Berrigan et al., Curr Rev Musculoskelet Med, 2024).
A 2021 randomized controlled trial published in Scientific Reports demonstrated that platelet dose is a critical factor in PRP outcomes for knee osteoarthritis. The study found that properly dosed PRP (10 billion platelets) produced significant improvements in pain, function, and walking distance compared to hyaluronic acid at one year follow-up (Bansal et al., Sci Rep, 2021). This reinforces what we see in practice: not all PRP is created equal, and preparation quality matters.
While the evidence is strong, it is important to note that PRP protocols vary between clinics, and not all PRP preparations are equal. Factors like platelet concentration, leukocyte content, and injection technique all influence outcomes. This is one reason why we track our own patient outcomes alongside published research.
Our Patient Outcome Registry
At Regenerative Performance, we have partnered with the DataBiologics outcome registry, a national database that tracks real-world results from regenerative medicine treatments. This gives us objective data on how our patients respond to treatment, not just what published studies suggest.
Our registry data across 376 cases over five years shows consistent patterns: more than three out of four patients (76.9%) achieve clinically meaningful pain relief, and 76.8% achieve meaningful improvement in daily function. Pain continues improving over time: a 45.1% average reduction in pain scores at 12 months, increasing to 57.6% at 18 months. Patients who seek treatment within 6 months of symptom onset see 84 to 93% responder rates. Published research supports sustained benefits at 18 months (Gobbi et al., KSSTA, 2015) and even out to 5 years (Di Martino et al., Am J Sports Med, 2019).
How Does PRP Compare to Steroid Injections?
Steroids provide faster but temporary relief and may degrade cartilage over time. PRP takes longer to work (4 to 12 weeks) but supports actual tissue repair with longer-lasting benefits. This is one of the most common questions we hear, and the answer involves important tradeoffs.
Steroid Injections
- Faster initial pain relief (within days)
- Works by suppressing all inflammation broadly
- Does not repair tissue
- Benefits fade over weeks to months
- Repeated use associated with accelerated cartilage breakdown (McAlindon et al., JAMA, 2017)
PRP Injections
- Gradual improvement over 4 to 12 weeks
- Modulates inflammation; preserves healing response
- Supports actual tissue repair via growth factors
- Benefits tend to last longer (12+ months)
- No risk of tissue degradation from the treatment itself
For patients with early to moderate joint degeneration, PRP offers a treatment approach that addresses the underlying problem rather than managing symptoms. For patients with more advanced joint disease, PRP may still provide benefit. In these situations, we often look at autologous stem cell therapy (bone marrow concentrate) as well, which can offer additional regenerative potential. You can learn more on our stem cell therapy page.
What Happens During PRP Treatment at Regenerative Performance?
Comprehensive 2-Hour Evaluation
Every new patient starts with a detailed 2-hour evaluation that includes a thorough history, hands-on physical examination with joint-specific provocation tests, tendon loading tests, and ligament stability tests, plus diagnostic ultrasound when indicated. We test the joint and surrounding tendons, ligaments, and nerves directly to determine whether they are the source of your pain, rather than relying solely on imaging.
The primary purpose of this evaluation is to identify the specific tissues causing your pain. This step is crucial because proper diagnosis is the single most important factor in regenerative treatment success.
Individualized Treatment Plan
Based on the evaluation, we determine whether you are a candidate for a PRP injection or another regenerative approach. From there, we develop an orthobiologic plan specific to your case, including which structures will be treated, the expected timeline, and your role in recovery.
Because the first three months after a PRP injection are the critical window where most healing occurs, we typically recommend supplements and peptides to support the healing process. Our goal is to give your body every advantage during that healing window.
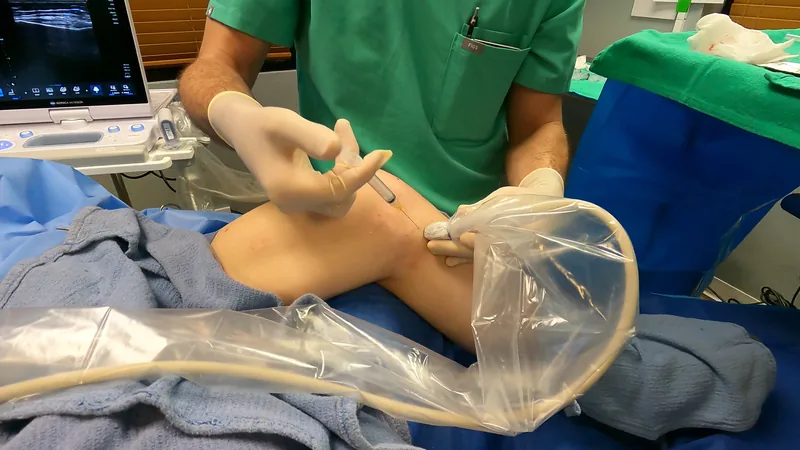
Ultrasound- and X-Ray-Guided PRP Injection
On your treatment day, we draw 120 to 300 mL of your blood, depending on how many structures we are treating. The preparation process typically takes one to one and a half hours because of how meticulous we are with processing. During this time, you relax in our IV lounge while we prepare your PRP to the highest standard.
We use ultrasound guidance for tendons, ligaments, and peri-articular structures, and combine ultrasound with x-ray guidance when treating intra-articular joints such as the SI joint or spinal facets. We treat each structure individually rather than relying on a single intra-articular injection.
Recovery and Follow-Up
After your injection, we recommend resting for the remainder of that day so your body can begin the healing process. Physical activity restrictions typically last 1 to 4 weeks, with a gradual return to full activity guided by your response. For most patients, we refer to a physical therapist who will design and adjust a rehabilitation plan specific to your treatment and goals.
In our clinic, most patients begin to notice changes within 4 weeks, with most of the improvement occurring over the first 3 months. Individual results may vary.
We schedule follow-up assessments to track your progress using our outcome registry, giving both you and our team objective data on how your treatment is working.

Schedule a comprehensive 2-hour evaluation for your chronic joint pain at our Gilbert, AZ clinic.
Who Is a Good Candidate for PRP?
PRP is typically a good fit for adults with chronic joint pain that has not responded to physical therapy, medications, cortisone injections, or even surgery. Our 2-hour evaluation is designed to confirm this for your specific situation.
Most patients who come to us share a similar profile. If you see yourself in the list below, PRP may be worth exploring.
- You have chronic joint pain that has not responded adequately to conservative treatment (physical therapy, medications, activity modification)
- You have imaging or clinical findings confirming structural damage (cartilage loss, tendon damage, ligament injury)
- You have realistic expectations about timeline and outcomes
- You do not have active infection, certain blood disorders, or conditions that would impair healing
- You are willing to follow the post-procedure rehabilitation protocol
- You are willing to invest in your health, as these are cash-pay procedures
During your evaluation, we will assess whether PRP is the right approach for your specific condition, or whether a different regenerative treatment (such as bone marrow concentrate) might be more appropriate.
If you are unsure whether orthobiologic injections like PRP or stem cell therapy are appropriate, or you are traveling from outside the Phoenix area, you can also call and ask about a brief 15 minute discovery call.
Frequently Asked Questions About PRP Injections
What types of joint pain does PRP treat?
PRP is used for a range of joint conditions including knee osteoarthritis, rotator cuff tendinopathy, hip osteoarthritis, tennis elbow, golfer's elbow, ankle sprains, plantar fasciitis, and sacroiliac joint dysfunction. The treatment is most effective for conditions involving tissue damage that has the biological capacity to respond to growth factor stimulation.
How is PRP different from cortisone shots?
Cortisone (steroid) injections suppress inflammation to provide temporary pain relief but do not repair tissue. PRP delivers growth factors that support actual tissue repair. Steroids work faster (days) but benefits fade; PRP works slower (weeks) but addresses the underlying damage. Repeated steroid injections may accelerate cartilage breakdown.
How many PRP treatments will I need?
Most patients require 1 to 3 treatments, depending on the severity and location of their condition. Some experience significant improvement after a single injection. Each patient responds differently, so treatment decisions are based on how you are progressing rather than a pre-sold series. We do not sell packages. Dr. Timmermans will discuss a specific treatment plan during your evaluation based on your diagnostic findings.
How long does it take to see results from PRP?
Most patients notice improvements within the first four weeks, with the majority of improvement occurring in the first twelve weeks. About 90% of the gains happen in the first three months. Full results are typically seen at six months. Patients who are actively working with a physical therapist may continue to see improvements beyond one year as they build on the foundation that PRP creates.
How long do PRP results last?
Many patients experience benefits lasting 12 months or longer, and our outcome registry data shows patients maintain improvement at their 18-month follow-up. Duration depends on the severity of your condition, activity level, and how well you follow the post-procedure plan including strengthening and lifestyle factors.
Is PRP covered by insurance?
PRP is not currently covered by most insurance plans. We provide transparent pricing during your evaluation visit so you know the full cost before committing to treatment. We work with Advance Care Card for patient financing to help make treatment accessible.
Is PRP safe?
Yes, PRP is safe. Because it uses your own blood, the risk of adverse reaction is very low. The most common side effects are temporary soreness and swelling at the injection site, which typically resolve within a few days. In our outcome registry, we have recorded zero severe treatment-related adverse events across 376 cases over five years.
What should I do to prepare for my PRP appointment?
Talk with your doctor about stopping anti-inflammatory medications (ibuprofen, naproxen, aspirin) at least 5 to 7 days before your procedure, as these can interfere with platelet function. We typically recommend a 12-hour fast before the blood draw because fasting increases growth factor content in your blood; discuss this with your doctor as well. Stay well hydrated in the days leading up to treatment and bring comfortable clothing that allows easy access to the treatment area.
Will I need physical therapy after PRP?
Physical therapy is an important part of the recovery process for most PRP patients. We coordinate with local physical therapists who understand regenerative medicine protocols. PT typically begins 2 to 4 weeks after injection, depending on the treatment area and your individual response.
How do you determine if I am a good candidate for PRP?
Dr. Timmermans determines candidacy during a two-hour evaluation that includes a detailed hands-on physical examination, imaging review, and diagnostic ultrasound. This evaluation identifies the specific structures causing your pain and determines whether PRP, bone marrow concentrate, or another approach is most appropriate for your condition.
Can PRP help avoid surgery?
For many patients, PRP provides sufficient improvement in pain and function to avoid or postpone surgical intervention. This depends on the severity of your condition. Our outcome registry helps us identify which patients are most likely to benefit from regenerative treatment versus those who may ultimately need surgical options.
How much does PRP cost in Gilbert, AZ?
PRP is not covered by insurance and is an out-of-pocket investment. We provide transparent pricing during your evaluation so you know the full cost before committing to treatment. We work with Advance Care Card for patient financing. Call 480-508-4226 to discuss pricing for your specific case.
What makes PRP at Regenerative Performance different from other clinics?
Three things set us apart. First, every treatment begins with a two-hour diagnostic evaluation, including a hands-on physical exam and diagnostic ultrasound, to identify the specific structures causing your pain. Most clinics skip this step. Second, we draw approximately 300 mL of blood and spend one to one and a half hours processing your PRP to achieve therapeutic platelet concentrations, significantly more than the standard 30-60 mL draw at most practices. Third, we track every patient outcome through the DataBiologics registry, giving us real data on how our patients respond rather than relying on assumptions.
Still have questions? The best way to get answers is a conversation. Call 480-508-4226.
Medical Disclaimer
PRP therapy is an autologous biologic treatment. The FDA regulates the devices used to prepare PRP but does not approve or disapprove PRP injections themselves as a drug or biologic product. Results vary by patient and condition. The information on this page is educational and does not constitute medical advice. We need to evaluate your specific situation before determining if PRP makes sense for you.
About Dr. Drew Timmermans
References
- Oeding JF, Varady NH, Fearington FW, et al. Platelet-Rich Plasma Versus Alternative Injections for Osteoarthritis of the Knee: A Systematic Review and Statistical Fragility Index-Based Meta-analysis of Randomized Controlled Trials. Am J Sports Med. 2024;52(10). PMID: 38420745.
- Bansal H, Leon J, Engel L, et al. Platelet-rich plasma (PRP) in osteoarthritis (OA) knee: Correct dose is the key to therapeutic efficacy. Sci Rep. 2021;11:3971. PMID: 33597586.
- McAlindon TE, LaValley MP, Harvey WF, et al. Effect of Intra-articular Triamcinolone vs Saline on Knee Cartilage Volume and Pain in Patients With Knee Osteoarthritis: A Randomized Clinical Trial. JAMA. 2017;317(19):1967-1975. PMID: 28510679.
- Tanpowpong T, et al. Effects of Platelet-Rich Plasma in Tear Size Reduction in Partial-Thickness Tear of the Supraspinatus Tendon Compared to Corticosteroids Injection. Sports Med Open. 2023. PMID: 36752928.
- Hewavithana PB, et al. Effectiveness of single intra-bursal injection of platelet-rich plasma against corticosteroid under ultrasonography guidance for shoulder impingement syndrome: a randomized clinical trial. Skeletal Radiol. 2024. PMID: 37266723.
- Berrigan W, Tao F, Kopcow J, et al. The Effect of Platelet Dose on Outcomes after Platelet Rich Plasma Injections for Musculoskeletal Conditions: A Systematic Review and Meta-Analysis. Curr Rev Musculoskelet Med. 2024. PMID: 39331322.
- Gobbi A, Lad D, Karnatzikos G. The effects of repeated intra-articular PRP injections on clinical outcomes of early osteoarthritis of the knee. Knee Surg Sports Traumatol Arthrosc. 2015;23(8):2170-2177. PMID: 24748286.
- Di Martino A, Di Matteo B, Papio T, et al. Platelet-Rich Plasma Versus Hyaluronic Acid Injections for the Treatment of Knee Osteoarthritis: Results at 5 Years of a Double-Blind, Randomized Controlled Trial. Am J Sports Med. 2019;47(2):347-354. PMID: 30545242.
- Nouri F, et al. Comparison between the effects of ultrasound guided intra-articular injections of PRP, HMWHA, and their combination in hip osteoarthritis. BMC Musculoskelet Disord. 2022. PMID: 36096771.
- Kumar S, et al. Comparison of Platelet-Rich Plasma and Corticosteroid Injections for Chronic Plantar Fasciitis: A Randomized Controlled Trial. Cureus. 2024. PMID: 38836136.
- Malahias MA, Nikolaou VS, Johnson EO, et al. Platelet-rich plasma ultrasound-guided injection in the treatment of carpal tunnel syndrome: A placebo-controlled clinical study. J Tissue Eng Regen Med. 2018. PMID: 28873284.
NOTE: This article provides general information to help the reader better understand regenerative medicine, nerve and musculoskeletal conditions, naturopathic approaches to pain, and related subjects. All content provided in this article, website, or any linked materials, including text, graphics, images, research, and outcomes, are not intended, and should not be used, as a substitute for direct medical advice, diagnosis, or treatment. Please always consult with a professional and licensed healthcare provider to discuss if any treatment is right for you.
Registry data from our single practice, powered by DataBiologics, is not a randomized clinical trial. Individual results may vary.
