Our Approach
A Workup-First, Individualized Approach to Hormone Therapy
Step 1: Comprehensive Evaluation
We start with a 120-minute visit to map your hormone picture, not guess at it. The goal is to understand how sex hormones, thyroid, adrenal output, sleep, stress, gut function, and nutrition are interacting in your body, and to identify which patterns are most likely driving the symptoms you came in with. Lab orders are tailored to your specific case rather than pulled from a template panel: sex hormones, full thyroid markers (TSH, free T3, free T4, antibodies, reverse T3 when indicated), adrenal patterns, metabolic markers, and nutrient status when patterns warrant it. You leave knowing exactly what we ordered and why.
Step 2: Individualized Plan
At your follow-up visit (typically 4 to 6 weeks after the initial evaluation, once labs return), the plan is built around what your body is actually missing or imbalanced, not a protocol applied to every patient. Dr. Myers walks through your results in plain language, shows how they fit your symptoms, and discusses the specific options that match your case.
If hormone therapy is appropriate, options we commonly discuss include:
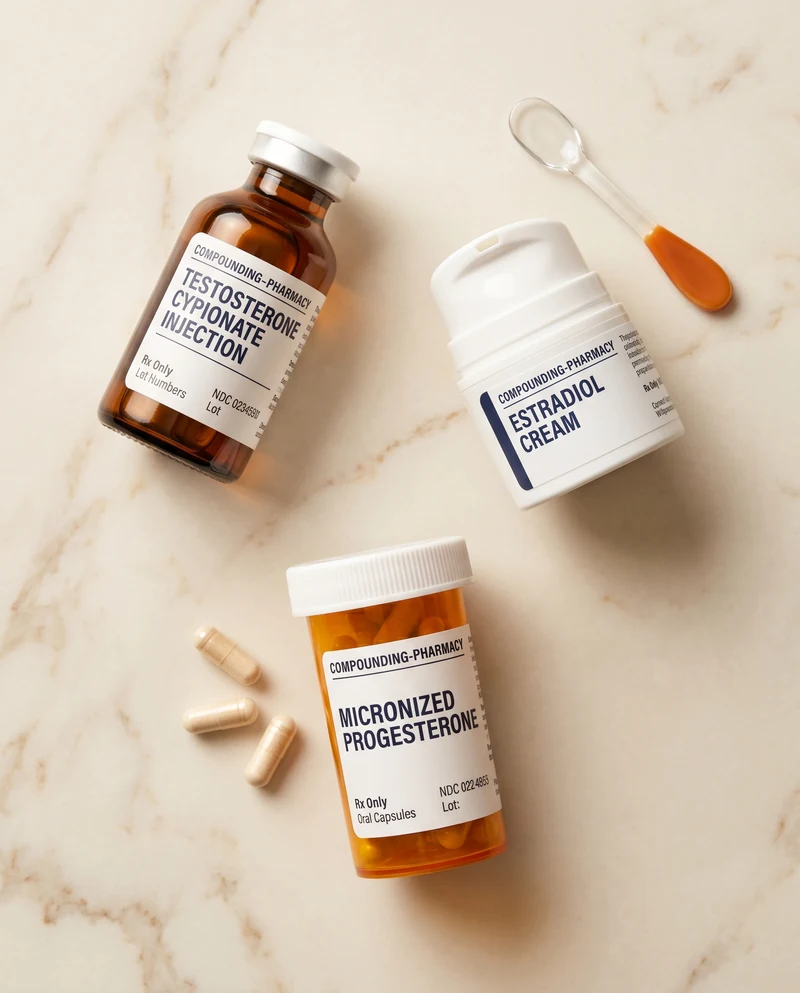
- Bioidentical estrogen and progesterone for appropriate women, prescribed as compounded creams, oral micronized progesterone, troches, or other adjustable preparations chosen to fit your symptoms and risk profile
- Testosterone replacement or optimization for appropriate men with documented low testosterone and for selected women whose symptoms and labs match. We use injections or topical preparations rather than pellets, which preserves dose flexibility and the ability to adjust quickly
- Thyroid and adrenal support when patterns warrant it, based on a full thyroid panel and adrenal markers rather than a single TSH or single cortisol value in isolation
- DHEA and pregnenolone as precursor hormones that feed downstream hormone pathways. When the body lacks the raw materials to produce its own estrogens, androgens, or cortisol effectively, supporting these precursors can sometimes restore better balance with lower dosing of the downstream hormones
- Nutrition, movement, sleep, and stress strategies so the hormones you are taking have the conditions to actually work, and so the upstream factors that influenced the imbalance get addressed alongside the prescription
Every plan includes non-hormonal strategies that support the same goals, including but not limited to herbs, specific vitamins and minerals, supplements, and peptides. The aim is to use the lowest effective hormone dose while addressing the upstream factors that influenced the imbalance in the first place.
Step 3: Ongoing Monitoring and Adjustment
Hormones are not set-and-forget. We schedule structured rechecks during the first 8 to 12 weeks once you start a plan, then move to a 6 to 12 month cadence once dosing is stable. At each recheck, dose, delivery route, and supporting strategies can be adjusted based on both your lab numbers and how you feel day to day.
The priority is to support how you function while respecting safety and long-term health. If a symptom pattern shifts, or labs show something we want to address, the plan shifts with it.